Post-Inflammatory Hyperpigmentation (PIH)
Understanding, preventing and treating dark marks after inflammation
The Skin Doctor
Who Is More at Risk?
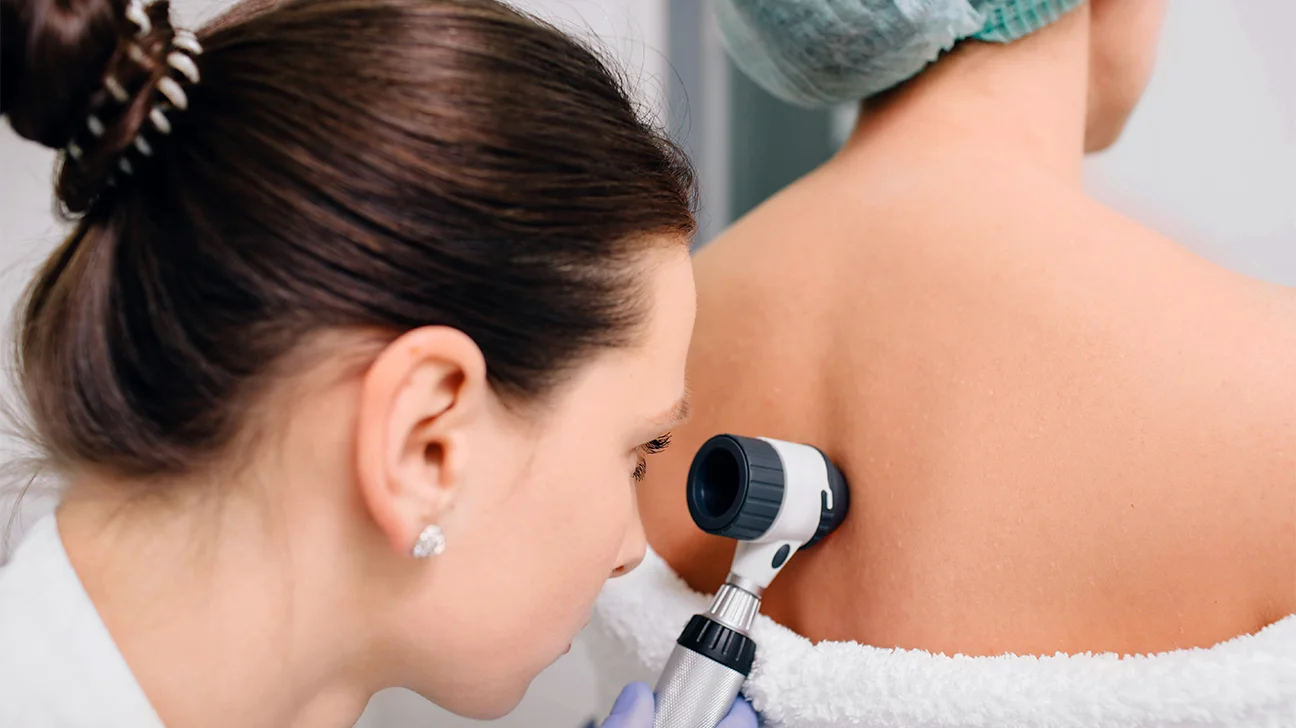
Medium to darker skin tones
Certain medications and supplements
Active inflammatory skin conditions
Conditions that increase inflammation raise the risk of PIH, including:
Acne, Eczema, Peri-oral / Peri-orificial Dermatitis, Seborrhoeic Dermatitis, and Psoriasis.
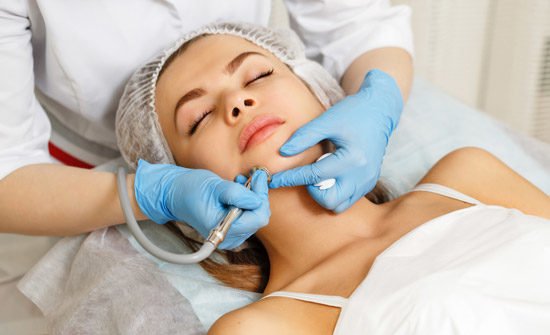
People prone to pigmentation
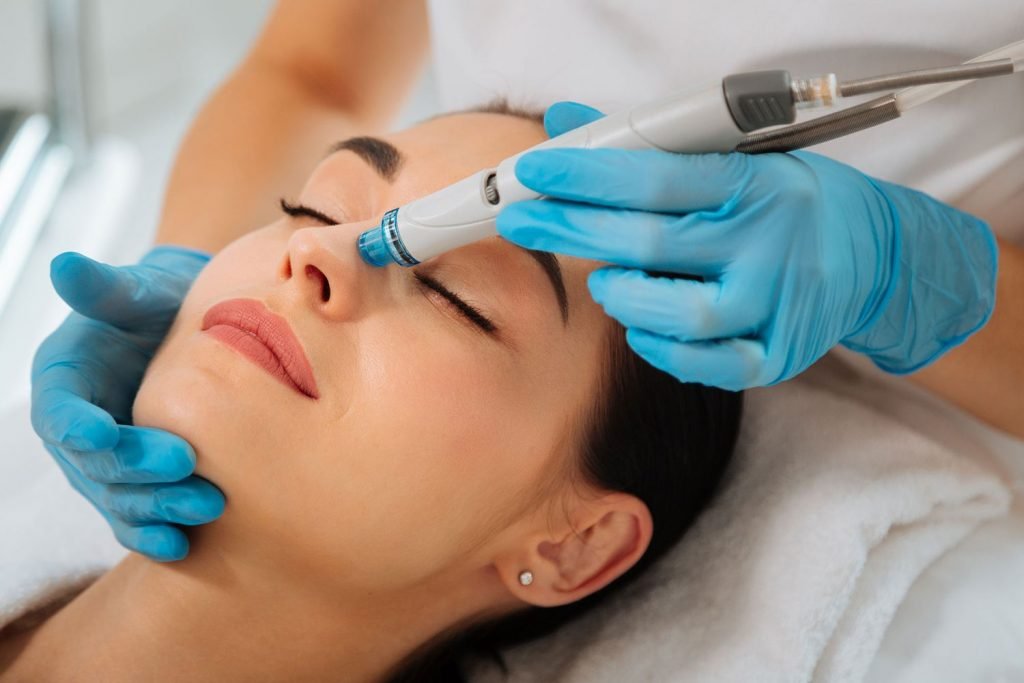
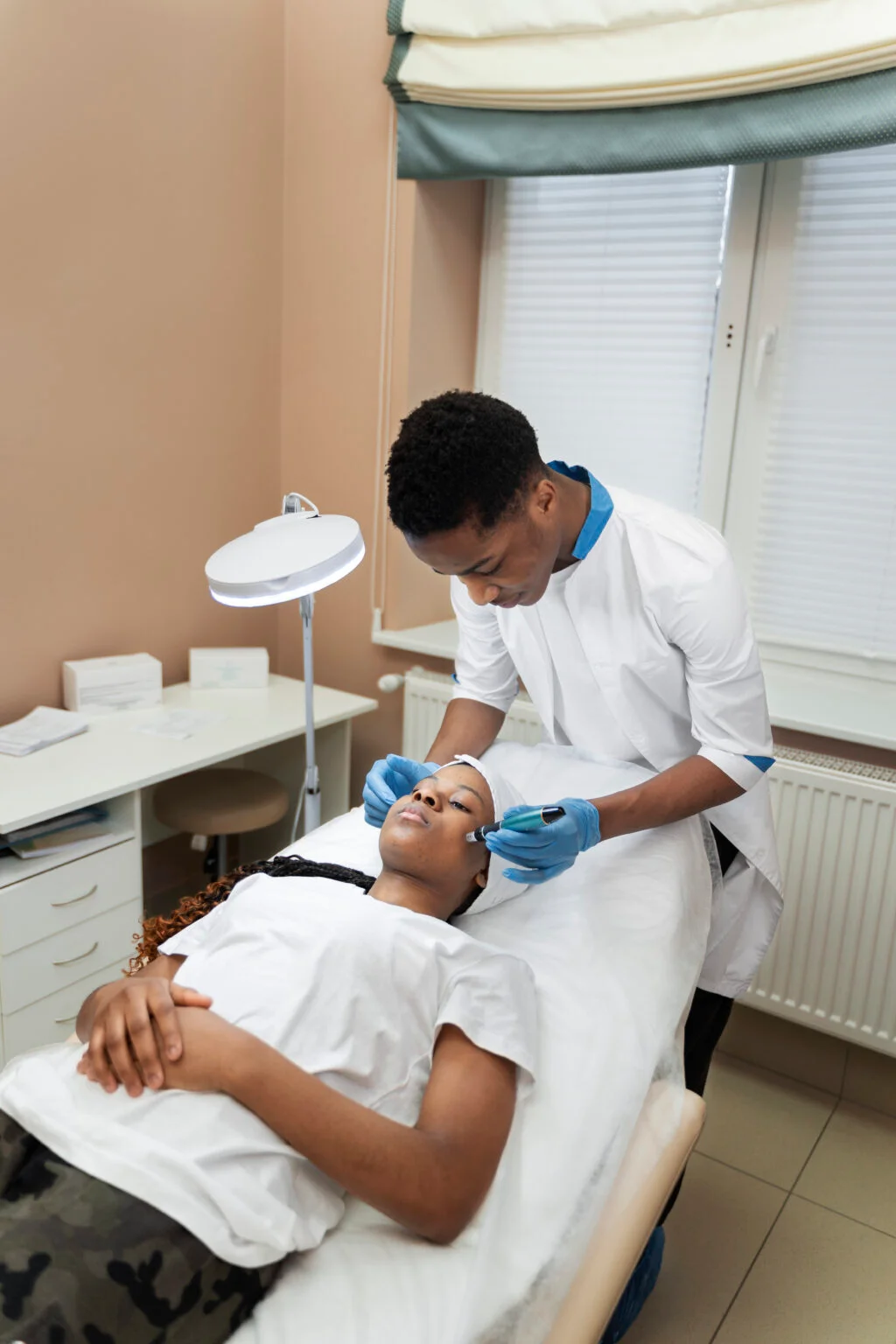
Heat- or trauma-based procedures
The Skin Doctor
Can PIH Be Prevented?
Sun protection
UV exposure amplifies pigmentation. Daily broad-spectrum SPF is essential before and after any treatment.
Avoiding photosensitising medications
Some medicines increase pigmentation risk with light-based procedures. As part of our safety process, patients confirm they are not taking common photosensitisers prior to treatment. For a comprehensive list, see Photosensitising Medications.
Pre-conditioning the skin
For higher-risk patients, Dr Chris may recommend:
- gentle pigment-suppressing agents (e.g. azelaic acid, niacinamide)
- strict moisturising routines to support the skin barrier
- avoiding irritation (retinoids, scrubs, harsh exfoliation) before procedures
Conservative treatment settings
Laser and energy-based treatments are adjusted to minimise thermal injury where appropriate.
Treating inflammation first
Stabilising acne, eczema or dermatitis reduces the inflammatory triggers that lead to PIH.
The Skin Doctor
Treatment Options for PIH
If PIH does occur, it is treatable. The most effective approach depends on skin type, cause, depth and severity of pigmentation.
At The Skin Doctor, treatment is tailored carefully — particularly for patients with procedure-related or higher-risk pigmentation.
Topical pigment-modulating treatments
Often first-line therapy, including:
- azelaic acid
- niacinamide (vitamin B3)
- vitamin C
- cysteamine
- hydroquinone (short-term, specialist-guided use only)
These help regulate melanocyte activity and fade pigmentation gradually.
Prescription-strength combinations
Compounded medical formulations may be used for more persistent PIH, particularly where laser is not appropriate.
Chemical peels
Gentle, medical-grade peels can assist exfoliation and pigment reduction, but must be selected cautiously to avoid further PIH.
Laser and light-based treatments
Used selectively and conservatively, low-fluence pigment-targeting lasers and LED therapy may help established PIH in suitable patients.
Improper or aggressive laser treatment can worsen PIH — which is why expertise and parameter selection are critical.
For laser-responsive pigmentation, see Pigmentation & Tattoo Removal.
Ongoing sun protection
Strict UV avoidance and sunscreen use are essential throughout recovery to maintain results.
How Long Does PIH Last?
- Mild PIH may fade within weeks
- More established pigmentation can persist for several months
Early, appropriate intervention often leads to faster and more complete clearing.
When Should I See a Doctor?
You should book an appointment if:
- pigmentation appears after a cosmetic treatment or laser session
- dark marks persist after acne or dermatitis
- you belong to a higher-risk skin group and are planning a procedure
- you want personalised guidance to reduce future PIH risk
We assess your skin thoroughly and develop a plan to both treat existing pigmentation and prevent recurrence.
Let's start
Book an Appointment
If you are concerned about PIH — or want to reduce your risk before upcoming treatments — our doctors can guide you safely.
